Poison control centers are fielding kratom calls at rates that would have seemed impossible just a decade ago, and the reasons behind the explosion reveal a troubling gap between what regulators allow and what doctors are witnessing in emergency rooms.
Quick Take
- Kratom-related poison center calls surged over 1,200% between 2015 and 2025, with 3,434 cases reported in 2025 alone
- Hospitalizations for kratom use jumped 1,150% for kratom alone and 1,300% when combined with other substances, with 60% of multi-substance cases requiring serious medical intervention
- The herb remains federally unregulated despite psychoactive properties that act on opioid receptors, making it available in gas stations and convenience stores nationwide
- A 2025 surge followed years of plateau, driven by increasingly potent formulations often mixed with addictive substances and antidepressants
What Doctors Are Actually Seeing
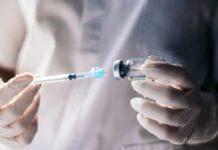
Emergency room physicians describe kratom patients presenting with wildly inconsistent symptoms, making diagnosis remarkably difficult. Some arrive nauseated and vomiting; others are dangerously sedated or confused. The unpredictability stems from kratom’s dual nature: at certain doses it stimulates, at others it sedates. What complicates matters further is the herb’s widespread availability in retail settings where consumers assume anything labeled natural carries minimal risk. Doctors emphasize this assumption is dangerously wrong. The substance acts directly on opioid receptors in the brain, producing genuine psychoactive effects alongside dependency potential and withdrawal symptoms comparable to opioid addiction.
The Numbers Tell a Startling Story
The trajectory of kratom exposures reveals a market that exploded quietly, then violently. From 2015 to 2019, reports climbed steadily. The years 2020 through 2024 showed relative stability, suggesting the market had plateaued. Then 2025 arrived. Poison control centers recorded 3,434 cases that year alone, representing a staggering 1,200% increase from the 258 cases in 2015. Hospitalizations for kratom use alone climbed 1,150%, from 43 to 538 cases. When combined with other substances, hospitalizations jumped 1,300%, from 40 to 549 cases. Deaths linked to kratom use totaled 233 across the entire decade, with 184 involving multiple substances. These figures suggest not just increased consumption, but increasingly dangerous formulations entering the market.
The Unregulated Potency Problem
Kratom occupies a regulatory blind spot. The federal government classifies it as a dietary supplement, which means manufacturers face minimal oversight regarding potency, purity, or accurate labeling. Traditional kratom from Southeast Asia involved chewing leaves for mild effects. Modern American kratom exists in concentrated pills, extracts, and powders of unknown strength. Vendors often add other compounds—stimulants, antidepressants, even addictive substances—without transparent disclosure. This adulteration drives the most severe outcomes. In 2025, roughly 60% of multi-substance kratom cases required hospitalization, indicating serious medical complications. The problem intensifies because these products are sold where consumers least expect danger: convenience stores, vape shops, and gas stations positioned as casual retail environments.
Who Bears the Greatest Risk
Kratom use skews heavily male, concentrated in the 20s to 30s age range, though cases are rising among 40- to 59-year-olds. Many users have histories of opioid use disorder, attempting self-medication with what they perceive as a natural, legal alternative. This population faces compounded risk because their opioid tolerance interacts unpredictably with kratom’s opioid-receptor activity. Additionally, those mixing kratom with other substances—alcohol, prescription medications, stimulants—face exponentially greater danger. Emergency physicians report that mixing kratom with other drugs produces complications ranging from respiratory distress to severe confusion to dangerously elevated heart rates. The challenge for healthcare providers is that kratom’s variable composition means they cannot predict patient responses or tailor treatment protocols effectively.
The Gap Between Availability and Awareness
Kratom’s legal status creates a peculiar paradox. The substance remains unscheduled at the federal level, making it completely legal to sell and purchase. Yet medical evidence increasingly demonstrates risks comparable to controlled substances. Poison control centers have seen the consequences escalate dramatically, particularly after 2025. Researchers and clinicians are calling for increased public education and heightened scrutiny of products sold as kratom. They emphasize that natural origin does not equal safety—a critical distinction lost on consumers browsing convenience store shelves. The medical community recognizes that without regulatory intervention or aggressive public awareness campaigns, poison centers and emergency departments will continue absorbing the consequences of a market operating without meaningful constraints on product safety or ingredient transparency.
The kratom crisis represents a modern version of an old problem: a substance marketed as benign gains popularity, concentrations increase, complications mount, and the regulatory system struggles to respond. The difference this time is that the data is clear, the medical consensus is firm, and the trajectory is accelerating. Whether policymakers act before more people face serious harm remains an open question.
Sources:
CDC MMWR: Kratom Exposure Reports and Hospitalizations
Powers Health: Kratom Cases Surging in U.S.
PMC: Kratom Use and Associated Health Outcomes